The sad truth is that most people who suffer from acne, know little to nothing about the type of acne they are dealing with — and then they wonder why the treatments they are using are not rendering any results! You may be living with fungal acne, and we know the solutions!
In this article we discuss the following:
- What is Fungal Acne?
- What does Fungal Acne Look Like?
- What Causes Fungal Acne?
- Fungal Acne vs Other Types of Acne
- How to Get Rid of Fungal Acne
- How to Get Rid of Malassezia Yeast
- Fungal Acne Product Ingredients to Avoid
- Fungal Acne Diet
- Fungal Acne Safe Products

What is Fungal Acne?
When any bodily condition is labeled “fungal”, you can rest assured that some kind of live yeast is at the center of the issue. Fungal acne is just that: a fungal infection caused by Malassezia yeast found in all skin.
This particular yeast is susceptible to growing in the beds of individual hair follicles when the conditions are just right (yeasts and funguses are live organisms — remember this!). When this happens, the follicles become inflamed, and fungal acne appears.
Scientifically speaking, fungal acne is not technically acne at all. Erik Pham, a health and wellness CEO, tells us that “Fungal acne isn’t really acne since it isn’t caused by pores and sebum. Instead, fungal acne is caused by a yeast-like infection that grew to the point that you could notice it.”
What Does Fungal Acne Look Like?
To better understand fungal acne from regular acne, we also spoke with Erica Suppa who was a cancer research scientist with GlaxoSmithKline. “Fungal acne are small bumps caused by yeast. We all have yeasts that naturally occur in our skin. These yeasts can also grow in hair follicles (which are found in our pores), and cause inflammation of the hair follicles. When inflammation of the hair follicles occurs, it causes the bumps referred to as fungal acne.”
Visually, fungal acne manifests physically as clusters of small, red bumps that do not tend to vary in size or shape. Occasionally, a few of the pimples can turn to small whiteheads, but this is not always guaranteed with fungus. Unlike regular types of acne, fungal acne is often a bit itchy.
Fungal Acne on Face
A fungal infection on face is the most common area to experience this kind of acne, however since Malassezia yeast is found across the entirety of the human skin, there is really no limit to where fungal acne can occur.
The face is most common because it is the part of our skin that is least covered from the elements of the external world. This will make more sense when we get into the numerous causes/triggers of fungal acne in human beings a little later on!
Fungal Acne on Forehead
When experiencing fungal acne on face, it is most likely that the spots are forming on the surface of the forehead. This area of the face is prone to skin infections, as there are less layers of tissue and fat compared to the lower part of the face. This is also where we come into most frequent contact with our hair, which can trigger excess sebum and yeast production.
Fungal Acne on Cheeks
The trouble with fungus is that it is naturally inclined to multiply, spread and “thrive”. So once fungal acne has started on the face, it is very difficult to stop it from spreading to other parts.
People suffering from facial fungal acne need to become extreme personal hygienists. Even sleeping on the same pillowcase twice could mean a new spread of fungus to a part of the face that was not yet infected. We’ll get into these hygiene tips more a little later in this piece — read on!
Fungal Acne on Chin
The chin is a naturally oily part of the face, and so excess sebum production is to be expected. For men, this area is particularly tricky as they are going to grow facial hair in this region, which puts them at an already heightened level of sebum production, creating higher risk for yeast!
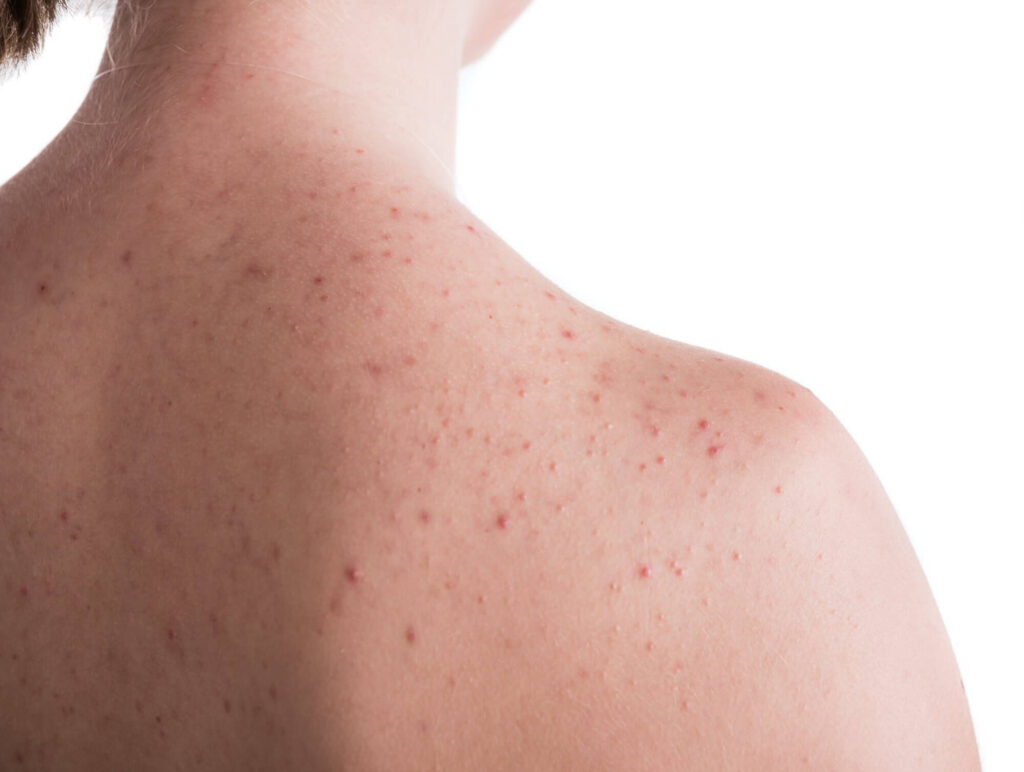
Fungal Acne on Back
“Bacne” (back-acne) is one of the most devastating conditions for the human spirit. People expect acne on the face, but when it chooses unusual regions one can be met with unkind gazes or diminished self-esteem.
Yes, fungal acne can occur on the back, and this can be a difficult region to treat due to things like reusing linen when sleeping, and reusing clothing until it needs to be washed.
Fungal Acne on Chest
Like the back, the chest is equally as susceptible to fungal acne breakouts. Usually, the one side triggers the other, thanks to the two scenarios we just mentioned. Sleeping in your bed with back acne, rolling over and making direct contact with the fungal residue on your chest, is likely going to trigger a spread of the spots.
Fungal Acne on Jawline
A surprising formation of this condition can occur solely along the jawline of the individual in question. When fungal acne is attacking the jawline and nowhere else, it can be a good indication that this individual has a self-care routine that totally stops once it reaches the chin.
The neck and jawline are too often neglected when it comes to personal hygiene and self care.
What Causes Fungal Acne?
Finally, the big question! Erica Suppa, the researcher we heard from earlier, has some points to make in this regard. “The main causes of fungal acne are most likely improper hygiene, medication you are taking, changes in your diet, or changes in your environment such as moving to a place with a relatively hot climate.”
Taking a look at each of these conditions in relation to your everyday life can be a great jumping off point for detecting your personal acne trigger. “This also means that treating fungal acne can be resolved based on its cause. If it’s improper hygiene, then simply wash your face more and bathe frequently. If it’s medications, then it’s best to consult your physician about this.” says Suppa.
How to Know if You Have Fungal Acne
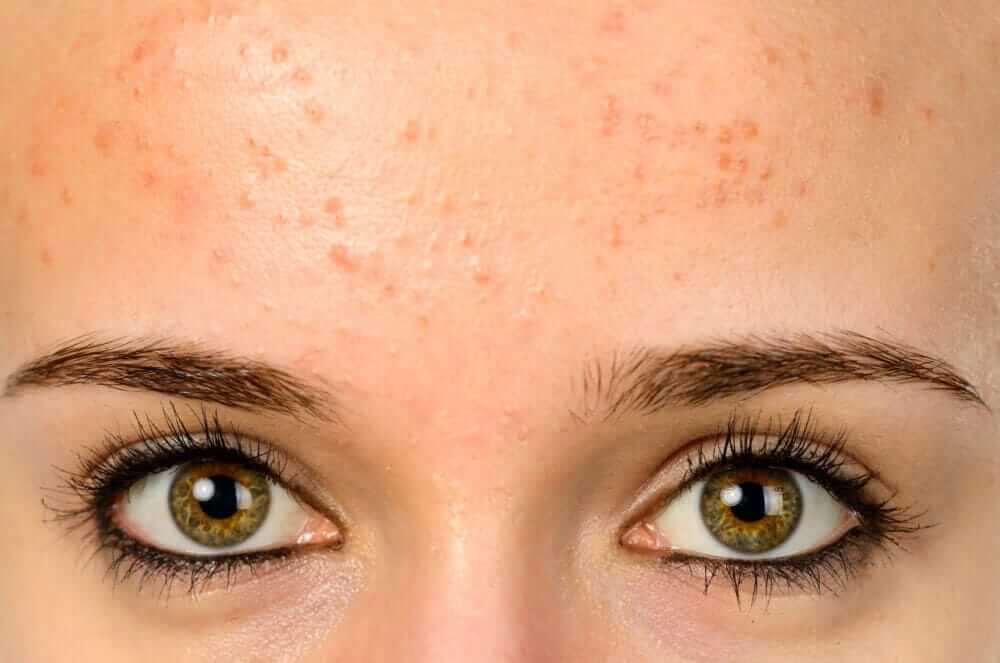
Only a dermatologist would be able to confirm the exact classification of your acne, however with fungal acne, self-diagnosis can be very easy if you simply use the following checklist as a point of reference. Ask yourself:
- Am I experiencing clusters of small, red bumps in similar sizes?
- Are some bumps forming whiteheads (but not all)?
- Is my skin slightly itchy?
- Is my acne spreading with contact?
- Have I been sweating more than usual recently?
- Am I taking medications?
- Has my hygiene routine taken a back seat recently?
- Has my diet been somewhat unhealthy recently?
Answering yes to three or more of the following questions is likely a good indication that you are dealing with active fungal acne.
Fungal Acne Symptoms
As mentioned, fungal acne symptoms are nothing too severe, with mild to intense itching being the most bothersome of the lot.
Other symptoms of fungal acne include the spots themselves, the emergence of whiteheads every so often, and undeniable inflammation of the affected region.
Can You Pop Fungal Acne?
It can be tempting to pop open any mild fungal acne, because it feels harmless and “worth a try”. For the most part, popping fungal acne is totally pointless because there is usually nothing inside of the little bumps. You’re simply putting yourself at risk for further infection and even scarring.
In the event of small whiteheads appearing within the acne clusters, popping can be even more tempting. Again, try to leave them alone. Adding any extra bacteria to the mix could create a lot more problems for you in the future, and totally derail your healing.
Does Fungal Acne Go Away?
Yes, fungal acne can go away on its own, but this process could take years due to the nature of fungus and yeasts. They want nothing more than to survive, and feed off of anything they come into contact with, which is why regular acne treatments just don’t work for this kind of condition!
With a targeted treatment regime specifically designed with fungal acne in mind, you could clear up your outbreaks within months or even weeks.
Fungal Acne vs Other Types of Acne
Fungal Acne vs Bacterial Acne
Fungal acne is most commonly confused with bacterial acne, as they can look very similar to the untrained eye. While they both exhibit whiteheads, the major difference between the two is that fungal acne’s whiteheads are always uniform in shape and size, whereas bacterial acne’s whiteheads will vary!
Bacterial acne also tends to involve a lot of blackheads, something that fungal acne will never produce.
Fungal Acne vs Closed Comedones
Another common error is assuming that fungal acne and closed comedones are the same thing. On the contrary, these could not be more opposite skin conditions.
Closed comedones are caused by a sebum overgrowth, not a yeast overgrowth! The individual follicles become completely blocked and whiteheads are produced. Unfortunately, this usually happens underneath the skin where we can’t actually see them! When they get big enough, the comedones are comparable to cysts and might exhibit a blackhead-type of opening in the skin where the build up is desperate to break free.
Fungal Acne vs Hormonal Acne
Hormonal acne and fungal acne should never really be confused. They are very different in that hormonal acne occurs on what seems to be a schedule, usually at a woman’s time of menstruation or during tangible hormonal spikes (imbalances).
Hormonal acne is also known as adult acne, and it usually only occurs on the lower region of the face, around the mouth and chin. Sometimes, hormonal acne can spread to just between the eyebrows, though this is more common in youngsters going through puberty and not adults.
Fungal Acne vs Regular Acne
Regular cases of acne are caused by oil and bacteria that block the pores and wreak havoc on the skin. Fungus is very rarely involved, and likewise in regular acne, oil and bacteria are never a contributing factor!
These polar opposites show why treatments for regular acne have no effect on fungal acne, which can be very frustrating to the individual who feels they are doing everything in their power to bring the condition under control. Most of the time, you’re simply doing it wrong!
How to Get Rid of Fungal Acne
We’ll now take you through exactly how to treat fungal acne; information that is still quite taboo and not nearly as widely known as it needs to be!
You’ll be pleasantly surprised to learn there are actually a number of different options on the market for the targeting of this kind of outbreak. We now know more about fungal acne than ever before in history, so the science behind the treatments is really starting to take off.
How to Treat Fungal Acne on Face
Treating fungal acne on the face means you’re going to have to make some changes to your existing self-care routine, at least just for a few weeks. What you’ve been doing up until this point is not serving you, and real change can only occur when real changes are implemented.
Again, Erica Suppa has some experience in this field, and tells us that “A great way to help fungal acne is to wash gently and apply an exfoliating serum, preferably one containing Mandelic Acid.” Woah, applying an acid solution to active acne? That’s not what we expected to hear.
“Mandelic Acid is derived from almonds and naturally exfoliates, but it is also naturally anti-fungal. In serum form, it will be highly concentrated and have a great amount of contact time with the skin, making it very effective in treating fungal acne.” explains Suppa. Acids derived from almonds are something we can certainly get behind!
Nizoral for Fungal Acne
Founder of Truism Fitness and qualified nutritionist, Jamie Hickey, is an advocate for strong anti fungal creams for the treatment of fungal acne. “Fungal acne can be treated with antifungals or oral isotretinoin (Accutane). This will kill the fungi present in your body and prevent it from coming back. These work well in mild cases but not severe ones.”
So what is the strongest antifungal cream? Well, according to Hickey, there are a lot of creams that you don’t want to self-prescribe without first consulting with a doctor. That said, Nizoral is a widely accessible brand that contains the fungal fighting formula of ketoconazole.
How to Use Nizoral for Fungal Acne
Using Nizoral for fungal acne is as easy as simply washing the skin twice daily with the solution, as you would any regular face wash. The ketoconazole within the wash will gradually lower the yeast levels in the skin, which will give your face a chance to reverse the condition.
Always use lukewarm water when washing with Nizoral. Too cold or too hot can cause further irritation, and we don’t have time for further irritation!
Clotrimazole for Fungal Acne
Clotrimazole is an anti-fungal cream that some individuals are using as a topical treatment for fungal conditions. The simultaneous downside and upside of this cream is that it is able to target many different kinds of funguses. This can be a benefit, but also a weakness in that it may be too mild for your particular kind of fungal infection.
Ketoconazole Cream 2% for Fungal Acne
Ketoconazole cream 2% is known worldwide as being a leading anti-fungal cream, used for treating everything from fungal acne to even the most serious cases of athlete’s foot.
As an over the counter product, this cream is easily accessible and doesn’t require a doctor’s prescription for use. The downside, you’ll need to coat your skin in the cream and leave it to sit like that for at least 3 hours before you can wash it off. This gives the solution the time to work its magic, but it can be incredibly inconvenient if you have places to be.
De La Cruz Sulfur Ointment Fungal Acne
In recent years, sulfur-based treatments have been making waves for the purpose of treating regular types of acne. Upon experimentation, people suffering from fungal acne started reporting that this product had worked for them as well, possibly due to the natural antibacterial properties that sulfur contains.
What’s also great is that it requires just a 10 to 15 minute treatment and then you can continue on with your day.
Honey for Fungal Acne
Another naturally antibacterial product is probably sitting in your kitchen pantry right now. Honey could be the key for your fungal acne, when mixed and applied properly.
A lot of people are not fond of the idea of ploughing their skin with chemicals in order to kill off a very natural organism: yeast. When honey is mixed with a paste-forming powder, such as turmeric, it can be applied to the skin like a mask and can gradually (and gently) bring the inflammation under control. Eventually, the conditions will no longer be favorable to the yeast, and it will starve into oblivion.
Turmeric has anti-inflammatory properties that compliment the honey. So too do spices such as cinnamon, ginger powder, cayenne pepper (not recommended for itching skin) and cloves.
Selsun Blue for Fungal Acne
There are some unfortunate people who actually experience a spread of malassezia folliculitis scalp. Yes, fungal acne within the follicles of head hair.
This unpleasant condition needs quick and effective action, as head hair is constantly producing sebum for the purpose of growth. Selsun Blue is an anti dandruff shampoo that many consumers around the world are reporting to be the key.
They claim to have seen results and improvement in their scalp acne after just a week of using the product. Worth knowing should your fungal acne ever come to this stage!
Head and Shoulders for Fungal Acne
Head and Shoulders is another anti dandruff shampoo that can be used for the purpose of getting scalp acne under control. We would say the former is a better one to try initially, but if you don’t find it effective enough then give this one a chance.
Head and Shoulders shampoos typically contain high levels of zinc, which is an effective means of treating all types of acne, not just fungal.
Vaseline for Fungal Acne
Despite what you were raised being told, Vaseline is not an acne-causing agent. On the contrary, there are a lot of people who have found Vaseline to be an invaluable companion throughout their acne journeys, be it for sealing in moisture or easing the itching sensations.
When it comes to fungal acne, we don’t recommend the Vaseline route. It’s not that it doesn’t have the potential to be effective, it’s more that it has higher potential to be devastating. Using Vaseline on fungal acne can produce reverse effects if the skin is even slightly moist at the time of application. Furthermore, the nature of Vaseline is that fingers are stuck in and out of the tub in order to use it, which usually means the entire jar is contaminated with bacteria after its first use.
Aloe vera is a more reliable alternative to Vaseline when it comes to fungal acne.
How to Get Rid of Malassezia Yeast
The aforementioned options aside, the best and most effective way to get rid of Malassezia yeast is to seek prescription malassezia treatment from a healthcare professional (HCP).
A targeted malassezia yeast treatment will be offered to you once your HCP has investigated the nature of your acne, and confirmed that it is indeed of fungal origin. They have access to creams and treatments that you won’t find online or OTC. For example, according to nutritionist Jim Hickey, second-generation topical treatments, such as Epidermofrance cream, can only be used when prescribed by a doctor!
How Long Does it Take to Cure Malassezia Folliculitis?
Let it be known, there is no quick fix for malassezia folliculitis. Anyone who promises you otherwise is probably going to take your money and run. Unfortunately, getting rid of this condition permanently requires time, patience and dedication.
On average, one can expect to see improvement in the condition of the skin between 1 and 2 months after starting a chosen treatment. Fungal acne can take upward of 6 months to a year to heal up entirely.
How Can I Treat Fungal Skin Infection Naturally?
This is where western medicine and homeopathic rituals come head to head, and get a little confusing. Fungal acne is complex in that the fungus itself is already a natural element, as is the yeast, so trying to eradicate them naturally can be extremely tricky.
You see, yeasts and fungi are naturally driven to eat and grow, just like every other living organism on Earth. Using natural products to treat this kind of infection could easily result in you simply feeding the organisms, instead of starving them.
That said, there are some natural products that holistic experts feel could hold the key for chemical-free treatments. They include apple cider vinegar, turmeric, garlic, aloe vera and powdered licorice.
Fungal Acne Product Ingredients to Avoid
Natural ingredients are not the only things that fungi and yeast feed off of. There are many other products that could be unknowingly fueling your acne, simply because the organisms themselves are partial to them!
If you’re suffering from fungal acne, you’ll want to temporarily remove any self-care products from your routine that contain the following:
- Oils (avocado oil, castor oil)
- Fatty acids (shea butter, cocoa butter)
- Polysorbate 20, 40, 60, 80
- Laurice acid or Myristic acid
- Subordinate isostearate
- Fermented ingredients
- Antibiotic creams
The website known as Folliculitis Scout offers a free online fungal acne ingredient checker, so that you can make the best choices for your skin through this time.
Fungal Acne Diet
When dealing with fungal acne, it’s not only what you put onto your skin that counts, it’s what you consume through your diet as well. Usually, fungal acne sets in when people become slightly immune compromised, perhaps after a cold or flu.
To heal the acne, your skincare routine needs to change, as does your diet. Fungi and yeast feed on carbohydrates and refined sugars, predominantly. Throughout treatment, you want to reduce your intake of both of these dietary components, and totally cut out sweets and soft drinks. Fruit sugars are acceptable provided they are digested with nothing else in the belly (digesting fruit and other foods together leads to fermentation in the gut and an excess of sugar).
Following any candida diet can be a good way of bringing your fungal acne under control.
Fungal Acne Safe Products
Adapting your fungal acne routine can feel daunting when all the focus lies on what you can’t use. Let’s take some time to look at safe fungal acne products that are not going to aggravate or spread your condition in using them.
Fungal Acne Safe Foundation
Covergirl + Olay Simply Ageless 3-In-1 Liquid Foundation

It’s okay (and totally natural) to want to cover up your fungal acne using foundation! And there are many safe ways of going about this. Firstly, please keep in mind that when you’re dealing with any kind of acne, you should never use any form of expired makeup on the face. Always purchase fresh, new products to limit bacterial exposure!
This foundation by Covergirl is a favorite amongst fungal acne sufferers around the world. It’s an incredibly gentle formula that also contains hyaluronic acid and vitamin C, which will help to prevent any scarring due to your spreading condition.
Antifungal Face Wash

Your chosen face wash can make or break your journey with fungal acne. When dealing with this condition, you need to temporarily switch out your usual product for something that is actually anti-fungal.
CeraVe has been a leading brand in treating different acne conditions for decades. Their SA Smoothing Cleanser is a favorite, and one that we highly recommended for mild to severe fungal breakouts. Why? It acts as a gentle exfoliator, which is essential if you ever want to enjoy clear skin in future!
Fungal Acne Safe Moisturizer
La Roche-Posay Toleriane Sensitive Fluide Protective Moisturizer

Your moisturizer will likely also need a facelift throughout your fungal acne treatment regime. It’s critical that you are not blocking the skin in any way; the pores need to breathe so that the fungus can be properly reached by other active products.
This moisturizer by La Roche-Posay is affordable and safe for skin that is suffocating with fungal acne. It contains no alarming ingredients that are known aggregators for this condition, and is totally oil-free (no oils allowed, remember?).
Fungal Acne Safe Sunscreen
EltaMD UV Clear Facial Sunscreen SPF 46 (Clear)

Just because you’re battling this hefty skin condition, doesn’t mean your protection and anti-aging rituals have to fall by the wayside. Even fungal infected skin needs to be kept safe from the sun, in fact arguably more so than healthy skin as it is considerably weaker thanks to the condition.
The trouble is that a lot of commercial sunscreens contain one or more of the ingredients on the fungal acne “no-no” list, so it can be difficult to find one that really works for your face!
This sunscreen by EltaMD is one that we know and trust. It’s notoriously light on the skin, and is made with breakouts in mind. It contains niacinamide (vitamin B3), hyaluronic acid and lactic acid, all safe compounds that work toward reducing inflammation (bonus!).
Please note that there is a tinted version of this sunscreen on offer as well, however this version is not safe for skin housing fungal acne. It’s important that you purchase the clear version!
Clay Mask for Fungal Acne
Lancer Clarifying Detox Mask with Green Tea + 3% Sulfur

Yes, you can still enjoy mask treatments even when fungal acne feels to be getting out of control! Clay masks are not going to feed yeasts and fungi, on account of the fact that clay itself is not a nutritional supplement, but rather a detoxifier.
Applying a safe clay mask to the skin every so often can work wonders for fungal acne, particularly if it’s this one by Lancer. Remember we looked at how sulfur could be the golden ticket to curing fungal acne gently? This wash-off clay mask is such in sulfur, alongside antioxidant rich green tea that will naturally reduce inflammation.
Skin suffering from fungal acne needs all the help it can get, so incorporating a clay mask into your schedule once or twice a week could really speed things along!
Fungal Acne Safe Concealer
NYX Can’t Stop Won’t Stop Contour Concealer

Sometimes foundation isn’t enough to give the kind of coverage that fungal acne truly needs. Using concealers underneath foundation can offer a slight improvement to both color and texture of the affected skin. Concealers are not a form of acne treatment, but if they give a person more confidence to face the world, then they are indeed healing in their own way.
The irony is that when it comes to fungal acne versus cosmetics, it’s usually the cheaper, less renowned brands that offer the safest solutions, because they aren’t packing harmful ingredients into their formulas for the hype!
NYX makes a fantastic concealer that retails for under $9 worldwide. It comes in every shade under the sun, so matching your tone needs is relatively simple! The ingredient list looks like a bit of a laboratory checklist, but it’s been dubbed one of the safest concealers on the market for this particular skin condition.
Best of all, this is an entirely vegan product, so you don’t need to worry about any animal proteins creeping in and feeding your yeast colonies. This is very important when it comes to any cosmetics used on fungal acne — stay alert!
Did You Enjoy This Article?
If you enjoyed this article, you might also like our articles discussing haircare, skincare, and oral care such as Best 11 Natural Mouthwash, Apple Cider Vinegar Shampoo, and Houttuynia Cordata (Heartleaf) and Skincare.



